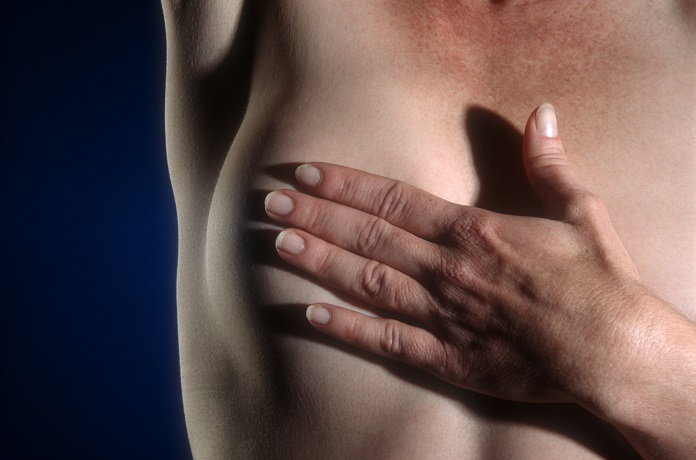
It’s the leading cause of death in women under 50 in the UK. But it’s not just women who suffer from this disease. We discuss seven signs and symptoms of breast cancer, what breast cancer screening involves, and some tips from two doctors who have had breast cancer.
Why do some people get breast cancer?
New research has shed light on the genetics of the disease, and scientists believe they are now closer than ever to discovering exactly why some women develop breast cancer and others don’t.
The OncoArray Consortium, which is the largest collective investigation on the genetics of the disease, has uncovered 65 new gene variants that appear to be responsible for increasing the risk. The results, published in science journals Nature and Natural Genetics, suggest around one in five women are at greater risk of contracting breast cancer because of mutations in their genes – which can be passed on through their families.
Scientists now believe a simple blood test could identify women who are at a third higher risk of later developing breast cancer. This could help them to establish a much earlier diagnosis.
While we may be closer than ever to understanding breast cancer’s origins, it’s still important to be vigilant when it comes to checking yourself regularly at home, no matter your age. According to Breast Cancer Now, 1 woman is diagnosed with breast cancer every 10 minutes, and around 55,000 women and 370 men are diagnosed with breast cancer every year in the UK. Yet many do not know the signs and symptoms that they need to look out for.
So we spoke to Dr Jasmine Just from Cancer Research UK, to find out what you should be looking out for.
Signs and symptoms of breast cancer
1. Breast lump

The first symptom of breast cancer for many women is a lump in their breast. But that shouldn’t be cause for immediate panic, as it may not necessarily be cancerous. Many of the symptoms of breast cancer, such as lumps, may in fact be caused by normal breast changes.
In fact, 9 out of 10 breast lumps are benign (not cancerous). If you do spot a lump, however, you should book in to see your GP straight away to put your fears at ease.
2. Change in size, shape or feel of a breast
The best thing to do is to regularly check your breasts to get a feel for what’s normal for you. Remember: everyone’s breasts are different shapes and sizes, so the more you check, the easier it will be to identify any changes.
You may find that your breast might look bigger or have a different shape than usual. It also might feel different, but many healthy women find that their breasts feel lumpy and tender before their period.
It is good to check your breasts in the shower. It can be useful to divide your breast into 4 quadrants to check thoroughly – don’t forget to check all the way up to your armpits. Knowing your breasts will help you identify the signs and symptoms of breast cancer early.
3. Breast pain
Breast pain is a very common issue for women which can be caused by hormonal changes, so it’s not a reason to panic. You might get pain in one or both breasts, which may come and go throughout the day. If it continues, make sure to see a doctor.

4. Skin changes
Skin changes are one of the more common signs and symptoms of breast cancer. Abnormal changes can include everything from puckering, dimpling, a rash, or redness of the skin of the breast. The skin might look like orange peel or the texture might feel different than usual.
This can be caused by other breast conditions, but you should get your doctor to check out anything that is not normal for you.
5. Change in the position of your nipple
Another important change to look out for is the positioning of your nipple. Warning signs include the nipple turning in or sinking into the breast – or it could just look or feel different to usual.
6. Fluid leaking from your nipple
Fluid leaking from a nipple in a woman who isn’t pregnant or breastfeeding can be a visual sign of cancer. But it can also be caused by other medical conditions – so make sure to consult a doctor if you’re unsure.
7. Inflammatory breast cancer symptoms
A rare type of breast cancer called inflammatory breast cancer can have different signs and symptoms to other types. Your whole breast might look red and inflamed and feel sore. The breast might also feel hard and the skin might have the texture of orange peel.
Most breast changes will not be cancer, however, it is important that you consult your GP to find out what’s causing the change.
Your GP will be able to examine your breasts and tell you if there is no need for further investigation, or if they think it’s necessary to refer you to a breast clinic. This doesn’t necessarily mean that you have breast cancer, it may just be that your doctor wants to conduct further tests are needed to find out what is going on.
What does breast cancer screening involve?
In the UK, women between the ages of 50 and 70 should be automatically invited to have a mammogram every three years.
About one in eight women in the UK are diagnosed with breast cancer in their lifetime, but the NHS screening system aims to catch the disease early, which gives women a much better chance of survival. So what should happen at a screening when you’re invited to have one?
Your invitation
If you’re registered with a GP, you’ll be invited for your first screening between your 50th and 53rd birthday, although in some areas there is a trial starting from the age of 47. Over 70, you’ll stop receiving invitations, but you can still request one. If you have breast implants you should let the staff know beforehand because they can make a mammography less effective.
2. Where is it done?
The X-ray, or mammogram, will be done at a specialist clinic or a mobile breast screening unit by a female practitioner. Take a partner or friend with you for support if you’re feeling anxious.
3. Symptoms
Before the exam, staff will ask about any breast problems you’ve had and explain the procedure. If you have any signs and symptoms of breast cancer, you should tell the staff now. You’ll need to undress to the waist for the exam.
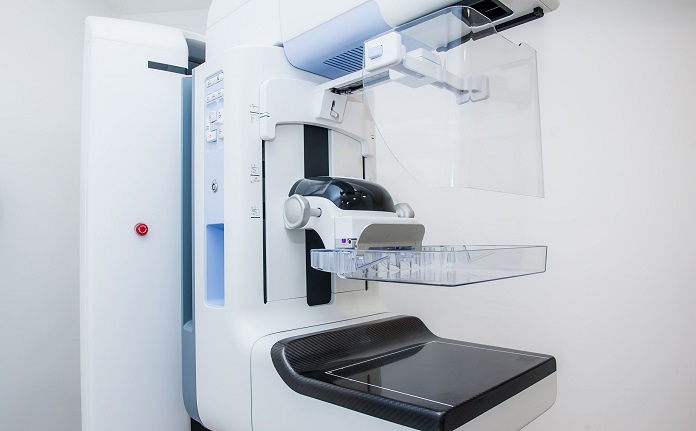
4. The X-ray
Your breasts will be X-rayed one at a time. Each breast is placed on the X-ray machine and a clear plastic plate will be gently lowered onto it. This is to compress and flatten the breast, which helps ensure a clear X-ray.
5. During the X-ray
The mammographer will go behind a screen while the X-rays are taken, and you’ll be asked to keep still for several seconds while two X-rays are taken of each breast – from above and from the side.
6. Is it painful?
Some women experience pain, while many just find the process a bit uncomfortable, but it only takes a few minutes and the compression doesn’t harm the breasts. The appointment will take less than half an hour overall.
7. Is it harmful?
Some people worry about the amount of radiation used in mammograms, but it’s a low dose, similar to the amount you’d get from a couple of long haul flights.
8. What happens afterwards?
The mammogram is checked for abnormalities and you and your GP will receive the results within two weeks.
For more information on what to do if you think you’ve been missed in the breast cancer screening error, visit Breast Cancer Care.
10 things everyone should know about breast cancer
Shock, disbelief and fear are just some of the emotions that might follow when a doctor tells you you’ve got breast cancer. But just because they’re usually on the other side of the consulting room, doctors aren’t immune to the disease either. Breast cancer surgeon Dr Liz O’Riordan, who was diagnosed with breast cancer in 2015, is on a mission to share her knowledge and insights with other patients.
She’s teamed up with fellow doctor-turned-breast-cancer-patient Professor Trisha Greenhalgh, to write the new book
The Complete Guide To Breast Cancer (available on Amazon). O’Riordan, 43, who was also diagnosed with a local recurrence of her breast cancer (meaning cancer had returned), and Greenhalgh, a GP and Oxford academic who was also diagnosed with breast cancer in 2015 at age 56, have both had chemotherapy and mastectomies.
At the start of their book, they say: “The moment you find out that you have breast cancer, your life changes forever. Because we have both had breast cancer we know, broadly speaking, what you are going through right now.”
Here are 10 things the pair think the one in eight UK women who develop breast cancer at some point in their life should know right from the start.

1. It’s not your fault
You can’t prevent breast cancer. There are some lifestyle factors, such as smoking, being overweight and binge-drinking after the menopause, that may play a role in increased risk, but slim teetotallers and healthy-living folk get breast cancer too.
“The biggest reason women get breast cancer is simply because they are women who are getting older,” says Greenhalgh. “Both are beyond your control. Stop feeling guilty – it’s not your fault.”
2. There are many new words to understand
There are several different types of breast cancers, depending on which bit of breast tissue the cancer grew in. Most cancers are ‘ductal’ because they grow in the milk ducts. There are other types, such as ‘lobular’ cancers which grow in the lobules (milk-producing glands) between the ducts.
Breast cancers are also described by the three hormones and chemicals they’re sensitive to. The first is oestrogen, and your cancer will either be ER-positive or ER-negative (it’s called ER because oestrogen is spelled ‘estrogen’ in America).
The second is progesterone, another female sex hormone, and your cancer will either be PR-positive or PR-negative. The third is a protein that makes cells grow, called HER2, and your cancer will either be HER2-positive or HER2-negative. If your cancer isn’t sensitive to any of these, it’s called ‘triple negative’.
3. Mastectomy isn’t the only option
O’Riordan, who blogs about her experiences at liz.oriordan.co.uk, explains that the surgery you need depends on the size of your cancer, and the size of your breast.
“Your surgeon can remove about a fifth of your breast tissue and leave you with a good cosmetic result. However, there are lots of techniques to help women with large tumours keep their breasts, such as a breast reduction, or using fat from your chest wall to fill in any gaps,” she says.
4. It’s OK to stay flat-chested
Anyone who needs a mastectomy should be offered a breast reconstruction, using either an implant or your own fat and muscle, says O’Riordan – but you don’t have to go for it.
“Some women, however, choose to stay flat-chested for lifestyle and personal reasons, and that’s OK too,” she stresses.
5. Not everyone needs chemotherapy
Only a third of women need chemotherapy, the authors point out. Most will have a simple lumpectomy, followed by a three-week course of radiotherapy.
If your cancer is sensitive to oestrogen, you’ll be given a tablet like tamoxifen or letrozole to lower the levels of oestrogen in your body as well. Although you’ll feel tired after treatment, you may only need a few weeks off work.
6. Chemotherapy isn’t fun, but you won’t remember it
Both women admit: “Chemotherapy is the thing no one wants, and we’ll be honest, it’s not fun. It takes five months in total, and you’ll feel poorly.”
However, they stress there are lots of things doctors can give you to help with side-effects, and there are also cookbooks and classes to help with eating when you lose your sense of taste. Try Ryan Riley’s book Life Kitchen (available on Amazon) which contains “recipes that are designed specifically to overpower the dulling effect of chemotherapy on the taste buds”.
In addition, there are ways to try and help prevent hair-loss during chemo, like wearing a cold-cap during treatment which cools the blood flow to your scalp. Most women who try this keep most of their hair, they say, “and six months after you’ve finished treatment, we promise you won’t remember how bad it was”.
7. Breast cancer can come back
Around 30% of women with breast cancer will get a recurrence in their lifetime says O’Riordan, who’s currently dealing with this herself. This can happen even after 10-20 years, she notes, and it’s important to know what the signs and symptoms of recurrent breast cancer are.
“Waiting to get the results of your yearly mammogram or any other test or scan is horrible – we call it ‘scanxiety’, and your family and friends may find it hard to understand what you’re feeling,” she says. “That’s where social media and online forums can be a godsend, so you can talk to other cancer patients who can give you the support and friendship you need.”
8. Exercise is important
There’s lots of evidence to show exercise is good for cancer patients, says Greenhalgh. As well as reducing the risk of a recurrence, it helps with the side-effects of treatments like chemotherapy.
Tablets like letrozole can cause osteoporosis, and weight-bearing exercise like walking and running can strengthen bones and help prevent it. And of course, exercise just helps you feel good, especially important when life gets tough.
9. You can get your sex life back
Breast cancer can have a devastating impact on your sex life, say the authors. You have to cope with an altered body image due to surgery and chemotherapy, and the menopause.
There are things you can do to make sex less painful – such as natural lubricants that you can get on prescription. Talk to your GP for help.
10. You can’t cure breast cancer with diet or supplements
There’s no evidence to show cutting any single food out or taking supplements will have a major impact on whether your cancer recurs, says Greenhalgh. Try to eat a healthy, balanced diet most of the time (as being overweight can increase the risk of a recurrence, as well as the risk of getting heart disease).
“However,” she adds, “you’ve had cancer, and if you want to drink bubbly or eat cake every once in a while, don’t feel guilty about indulging yourself!”
You may also be interested in…
This article may include affiliate links to products and services where we may receive a small fee to support the running of this site if you make a purchase or is a sponsored article from one of our select editorial partners providing valuable advice and information to our readers.