It’s been dubbed one of the fastest growing health crises of our time, with 4.7 million people in the UK suffering from diabetes. Yet despite the condition being so common, there’s a huge lack of understanding around exactly what the disease is, and how it’s triggered and treated.
In many cases, this serious condition is largely preventable. Yet the number of people diagnosed continues to grow, and here in the UK, figures have more than doubled in the last 20 years, according to analysis by Diabetes UK.
What is diabetes?
Diabetes is defined as a group of serious, lifelong metabolic disorders that causes a person’s blood sugar level to become too high.
Professor Francesco Rubino, a consultant surgeon at the London Bridge Hospital Metabolic and Bariatric Centre (HCA Healthcare UK), outlines six key facts everyone should know about diabetes…
1. There are two types of diabetes
“There two main types of diabetes, Type 1 and Type 2. Although both types are characterised by an elevation of glucose (sugar) in the blood, Type 1 and Type 2 diabetes differ in many ways. ,” explains Rubino.
Type 1 – “Type 1 is an autoimmune condition where the pancreas can’t produce insulin, a hormone that controls blood sugar levels. Hence, patients require injections of insulin or special insulin pumps.
Type 2 – “With Type 2, the pancreas can usually produce insulin, but the amount produced isn’t enough, as the body’s cells are resistant to the effects of insulin. In addition to elevating blood sugar, such resistance can cause additional metabolic dysfunction, which explains why Type 2 diabetes is often associated with other conditions such as high blood pressure, increased blood lipid levels, and fat deposition in the liver. Although Type 2 diabetes is initially treated by diet and oral drugs, some patients may eventually require insulin as the ability of the pancreas to make it deteriorates over time due to the hard work required to overcome insulin resistance.”
“Type 1 usually begins in childhood, but can also occur later in life,” Rubino adds. “Although Type 2 is more often diagnosed in adult life, over the last two decades there’s been an increasing prevalence in adolescents.”
Type 2 diabetes is far more common than Type 1, and the NHS estimates that around 90% of all adults with diabetes have Type 2.
2. Many people don’t know they have diabetes
“Up to 549,000 people [are] thought to be living with the condition undiagnosed in the UK alone.”
3. Symptoms aren’t always obvious
“Many people have Type 2 diabetes without realising, because symptoms aren’t always obvious, and don’t necessarily make you feel unwell,” says Rubino.
He notes that symptoms include: “Feeling tired during the day, particularly after meals; increased hunger, particularly after eating; urinating more frequently, particularly during the night; feeling unusually thirsty; blurred vision; itching of the skin; slow healing cuts or wounds; regular yeast infections; sudden weight loss or loss of muscle mass.”
“Up to 549,000 people [are] thought to be living with the condition undiagnosed in the UK alone.”
4. There are risk factors for anyone when it comes to Type 2 diabetes
“Anyone can develop Type 2 diabetes, but there are a number of factors which make some people more susceptible to the disease than others,” says Rubino. These include:
- Obesity: A high BMI is strongly associated with increased risk of developing Type 2 diabetes. The risk is highest when fatty tissue is mostly located around the abdominal area. For reasons that aren’t entirely understood, this particular type of fat distribution is strongly associated with insulin resistance.
- Age: Risk can increase with age, as people over 40 become less active, carry more fat and tend to become less sensitive to the action of insulin
- Ethnicity: Type 2 diabetes is more likely to occur in people of South Asian descent and African-Caribbean or Black African descent, for reasons unknown.
- Genes: Type 2 diabetes is more likely to occur if there’s a history of disease in a parent, brother or sister.
- High blood pressure: A history of high blood pressure has also been known to put people more at risk of developing the disease.
- Polycystic ovary syndrome (PCOS): PCOS is associated with insulin resistance, meaning higher levels of insulin circulate in the blood – thus increasing the risk of Type 2 diabetes.
5. Type 2 diabetes can be simple to diagnose
Rubino says “Type 2 diabetes can be diagnosed using a blood test, which gives an indication of the average blood sugar level for the past two to three months.”
“A combination of diet, exercise and medication are often prescribed to patients with Type 2 diabetes. and in many cases these can bring blood sugar under control,” he adds.
6. Surgery isn’t necessarily a last resort
“Traditionally, bariatric (weight-loss) surgery has been seen as a ‘last resort’ in the management of obesity and diabetes,” notes Rubino, however, “we now know the stomach and small bowel play a crucial role in the regulation of both the production of insulin and the sensitivity of the body to insulin, explaining the dramatic effects of gastrointestinal surgery on diabetes.
“For this reason, traditional weight-loss procedures are being repurposed as a diabetes treatment, known as metabolic surgery.”
“As we change the anatomy of the stomach and/or the intestine, we also change the signals from these organs, which are involved in the control of metabolic functions. In addition to improving blood sugar levels, metabolic surgery can also help the body to better regulate hunger, satiety and content of fat in the liver,” Rubino explains.
“Studies show about half of patients with Type 2 diabetes who have keyhole metabolic surgery can discontinue all glucose-lowering drugs while maintaining normal levels of sugar in their blood for many years, and possibly lifelong.”
7. Untreated diabetes can lead to serious complications
“Type 2 diabetes is a condition that gradually progresses and worsens over time,” Rubino warns. “If it goes untreated, the high blood sugar can impact various cells and organs in the body, potentially resulting in complications such as kidney damage, dialysis, eye damage, and an increased risk of heart disease and stroke.”
“Untreated diabetes can also affect the feet, triggering diabetic foot disease, which can lead to numbness and even gangrene and amputation,” he adds. “In addition, high levels of sugar in the blood could potentially result in a coma or, in very extreme cases, potential death.
“It’s therefore vital that people are aware of the symptoms, so they can be diagnosed and treated as soon as possible,” stresses Rubino.
What are the symptoms of diabetes?
Here are some of the most common warning signs to look out for…
1. Unexplained weight loss

If you haven’t made any changes to your diet or exercise routine, but you’ve noticed a significant drop in your weight (losing a few pounds here or there is normal), it could be a sign that something isn’t quite right.
In people with diabetes, insufficient insulin prevents the body from getting glucose from the blood into the cells to use as energy, so as an alternative, it burns fat and muscle instead.
2. Recurring thrush
People with diabetes are more likely to suffer from yeast infections because they have more sugar in their bodies. High blood sugar levels are one of the main causes of thrush, along with a weakened immune system, which is also common in people with diabetes.
3. Needing to urinate more frequently

Frequent urination is one of the major signs of both Type 1 and Type 2 Diabetes. This irritating symptom usually occurs because sugar builds up in your blood, and your kidneys are forced to work overtime to filter and absorb it. As the kidneys struggle to keep up with the rate of work, the sugar is excreted into your urine, causing you to need the toilet.
4. Feeling thirsty
Noticed you’re in need of a drink more than usual? If you have a thirst you can’t quench, it might be down to diabetes. As the body urinates more frequently to get rid of the excess sugar in your system, it triggers the thirst reflex to help replace the fluid you’re losing.
5. Blurred vision
As well as your kidneys, diabetes can also affect your eyesight too. High levels of blood sugar pull fluid from your tissues, including the lenses of your eyes, which makes it harder for your eyes to focus.
6. Fatigue

Glucose, along with dehydration, can make your feel really sluggish and groggy, making it difficult for people who suffer from Diabetes to feel energised in the morning. Fatigue is feeling very tired most, or all, of the time.
7. Slow-healing wounds
Research has found a link between high levels of glucose and wounds that are slower to heal. While minor cuts and scrapes are a part of everyday life, they can be more serious for someone with diabetes, as wounds that do not heal well can become infected, leading to serious health issues.
8. Darkened skin
Darkened skin, or to use its proper name, Acanthosis Nigricans, is frequently found in people with insulin resistance – common for type 2 diabetics. “It’s like a dark, velvety pigmentation,” says Dowling, “which you would typically see under the armpits or at the back of the neck.” Perfectly healthy people can contract the condition – but it’s worth seeing your doctor all the same.
If you have any symptoms of diabetes, there’s no immediate reason to panic, but you should contact your GP and get tested if you’re concerned. It doesn’t necessarily mean you have diabetes, but it’s worth ruling out, as early diagnosis means you can access treatment sooner, which is vital to reduce the chances of developing serious complications.
What are the symptoms of diabetes in children?
Rates of type 2 diabetes in children and young adults have skyrocketed to the highest ever recorded – here’s how to spot the telltale signs
Let’s begin with some bad news – the signs of type 2 diabetes are almost all subtle.
“In type 1 diabetes, symptoms are pretty classic and obvious,” says Libby Dowling, Diabetes UK’s senior clinical adviser, “in type 2 diabetes, they’re the same symptoms – but unfortunately, they’re much more subtle and often missed.”
Parents, adds Dowling, are best-placed to know what is normal for their child, and should consider a check-up if there’s a major deviation from it. Symptoms vary for different children and different ages, so don’t blame yourself if you miss things.
Link between the disease and mental health
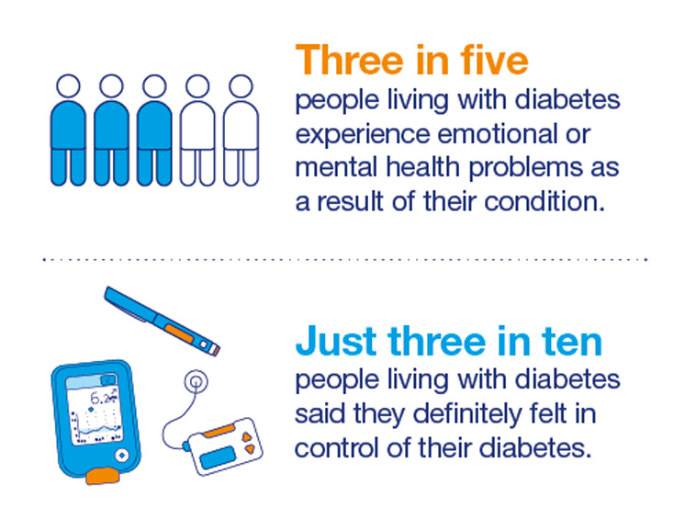
Diabetes may be a physical condition, but the mental impact can be huge. A study of sufferers by Diabetes UK, found 64% of those questioned often felt down because of their diabetes, with some suffering from problems such as depression and anxiety, while a third of respondents said diabetes had got in the way of them or a family member doing things they wanted to do in the previous week.
Chris Askew, Diabetes UK chief executive, says: “This new research brings to light the isolation that can come from managing an invisible condition, and how detrimental living with diabetes can be to a person’s emotional wellbeing without the right support.”
The charity is calling for more provision of psychological support for those living with the condition, which affects more than 4.5 million people in the UK, and can lead to heart disease, stroke, kidney failure and lower limb amputations. Here’s what you need to know.
Mental health problems are common in people with diabetes
“Mental health and diabetes are rarely discussed,” says Douglas Twenefour, deputy head of care at Diabetes UK, “but it’s common in people with diabetes.
“Depression is twice as common in people with diabetes as in the general population, and around 40% of people with diabetes experience poor psychological wellbeing, often directly related to the demands of living with diabetes.”
Lis Warren was diagnosed with Type 1 diabetes in 1965 when she was 13 years old, and suffered from an eating disorder as a result of living with the disease. “When I was diagnosed, diabetes was seen as a medical condition, but there was little understanding of the effect it has on mental health, so psychological support was unavailable. I started struggling with food when I was a teenager. When I look back now, I had an eating disorder. I was having seizures from low blood sugar when I was routinely eating insufficient carbohydrate to lose weight – I didn’t speak to anyone about how diabetes had affected my mental health for 40 years.”
Mental health issues can stop sufferers self-managing their diabetes
Managing the condition is hugely important for people suffering from both Type 1 and Type 2 diabetes. Patients needs to continually monitor their blood sugar levels, blood pressure and cholesterol levels. A mild case of hypoglycemia (caused by blood glucose levels dropping) can usually be treated by eating or drinking a fast acting carbohydrate. But severe hypoglycemia requires medical treatment and, while rare, can lead to coma and death.
“It is important that people with diabetes who have mental health problems get support,” says Douglas. “Mental health problems among people with diabetes can reduce their ability and motivation to self-manage, leading to poorer quality of life and a greater likelihood of complications and early death.”

Blaming overweight people for their Type 2 diabetes can be harmful
Unlike Type 1 diabetes, Type 2 is linked to obesity, which means mean making positive lifestyle changes – such as eating a healthy diet, exercising and stopping smoking – can help prevent people from developing the disease. But this may not be the only reason people develop Type 2 diabetes.
“People should also refrain from blaming people with diabetes,” Douglas explains. “This is especially the case for people with Type 2 diabetes. Although we know that weight and lifestyle is a significant factor in Type 2 diabetes, there are still a lot of things we do not fully know about the condition. There are a lot more factors associated with Type 2 diabetes, such as ethnicity, family history and age, so the link between obesity and diabetes needs to be carefully explained.”
Education is vital to combat mental health issues
Knowledge is power when it comes to living with either type of diabetes. Douglas says: “People with diabetes need access to the right information and advice, at diagnosis and throughout their lives. We would advise that people with diabetes go on educational programmes, like DAFNE or DESMOND, to help them experiment, learn and take action to manage their condition well.
“Peer-to-peer and online forums, like Diabetes UK’s support forum, are also a great way to talk to other people with diabetes. Sharing and finding out more about the condition with other people is a great way to get support.”
He adds: “It is very important for loved ones to understand how diabetes impacts on their day-to-day life and know their individual needs.”
Read more: How to lose weight in your 20s, 30s and 40s